“第二次机会”应用程序检测到阿片类药物过量及其前体
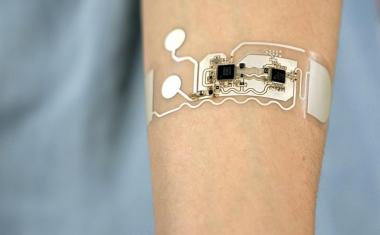
研究人员开发了一个应用程序,该应用程序使用声纳来监测某人的呼吸速度和感觉,何时发生了阿片类药物过量。
At least 115 people die every day in the U.S. after overdosing on opioids, according to the National Institute on Drug Abuse. And in 2016, illegal injectable opioids became the most common drug involved in overdose-related deaths. This spike has led to a national public health crisis and epidemic. During an overdose, a person breathes slower or stops breathing altogether. These symptoms are reversible with the drug naloxone if caught in time. But people who use opioids by themselves have no way of asking for help in the event of an overdose.
Researchers at the University of Washington have developed a cellphone app, called Second Chance, that uses sonar to monitor someone’s breathing rate and sense when an opioid overdose has occurred. The app accurately detects overdose-related symptoms about 90 percent of the time and can track someone’s breathing from up to 3 feet away. “The idea is that people can use the app during opioid use so that if they overdose, the phone can potentially connect them to a friend or emergency services to provide naloxone,” said co-corresponding author Shyam Gollakota, an associate professor in the UW’s Paul G. Allen School of Computer Science & Engineering. “Here we show that we have created an algorithm for a smartphone that is capable of detecting overdoses by monitoring how someone’s breathing changes before and after opioid use.”
Detecting precursors
第二次机会应用程序将声音从手机传递到人们的胸部,然后监视声波返回手机的方式,以寻找特定的呼吸模式。“We’re looking for two main precursors to opioid overdose: when a person stops breathing, or when a person’s breathing rate is seven breaths per minute or lower,” said co-corresponding author Dr. Jacob Sunshine, an assistant professor of anesthesiology and pain medicine at the UW School of Medicine. “Less than eight breaths per minute is a common cutoff point in a hospital that would trigger people to go to the bedside and make sure a patient is OK.”
In addition to watching breathing, Second Chance also monitors how people move. “People aren’t always perfectly still while they’re injecting drugs, so we want to still be able to track their breathing as they’re moving around,” said lead author Rajalakshmi Nandakumar, a doctoral student in the Allen School. “We can also look for characteristic motions during opioid overdose, like if someone’s head slumps or nods off.”

为了能够使用现实世界数据设计和测试应用程序背后的算法,研究人员与加拿大温哥华的Insite监督注射设施合作。Insite是北美第一个法律监督消费地点。作为研究的一部分,Insite的参与者在其胸部戴着监视器,这些监视器也跟踪呼吸速度。Nandakumar说:“我们要求参与者像往常一样准备他们的药物,但后来我们对他们进行了一分钟的注释,以便算法可以获得其呼吸率的基线价值。”“在获得基线后,我们在注射过程中继续进行监测,然后在五分钟后进行监测,因为那是发生过量症状的窗口。”
在测试该算法的94名参与者中,有47个呼吸速度为每分钟7次或较慢的呼吸,有49个呼吸在很大一段时间内停止呼吸,两人经历了过量事件,需要氧气,通风和/或纳洛酮治疗。平均而言,该算法正确地识别出预示了90%时间的呼吸问题。
The researchers also wanted to make sure the algorithm could detect actual overdose events, because these occur infrequently at Insite. The researchers worked with anesthesiology teams at UW Medical Center to “simulate” overdoses in an operating room, allowing the app to monitor people and detect when they stop breathing. “When patients undergo anesthesia, they experience much of the same physiology that people experience when they’re having an overdose,” Sunshine said. “Nothing happens when people experience this event in the operating room because they’re receiving oxygen and they are under the care of an anesthesiology team. But this is a unique environment to capture difficult-to-reproduce data to help further refine the algorithms for what it looks like when someone has an acute overdose.”

为了模拟,团队招募了接受以前计划的选修手术的健康参与者。在提供知情同意后,患者随后接受了标准麻醉药物,导致30秒钟的呼吸速度慢或没有呼吸,这些事件被设备捕获。该算法正确地预测了20种模拟过量药物中的19个。对于一种情况,这是错误的,患者的呼吸速度刚好超过算法的阈值。
目前,第二次机会只是监视使用它的人。团队最终希望该应用程序与他们互动。Gollakota说:“当该应用检测到减少或没有呼吸时,我们希望发出警报要求该人与之互动。”“那么,如果该人没有与之互动,那就是我们说:‘好吧,这是我们需要提醒某人的阶段,”手机可以与纳洛酮联系。”
研究人员正在申请FDA批准,并计划通过称为Sound Life Sciences,Inc。的UW旋转来商业化这项技术。虽然该应用程序可用于所有形式的阿片类药物使用,但团队警告说,现在他们只对其进行了测试。非法注射阿片类药物的使用是因为这些过量的死亡是最常见的。Sunshine说:“我们正在经历阿片类药物使用的死亡人数前所未有的流行病,这是不幸的,因为如果及时发现这些过量药物是完全可逆的现象。”“该项目的目的是尝试将经常经历过量服用的人与可以挽救生命的已知疗法联系起来。我们希望通过保持人们更安全,他们最终可以接受长期治疗。”
来源:华盛顿大学